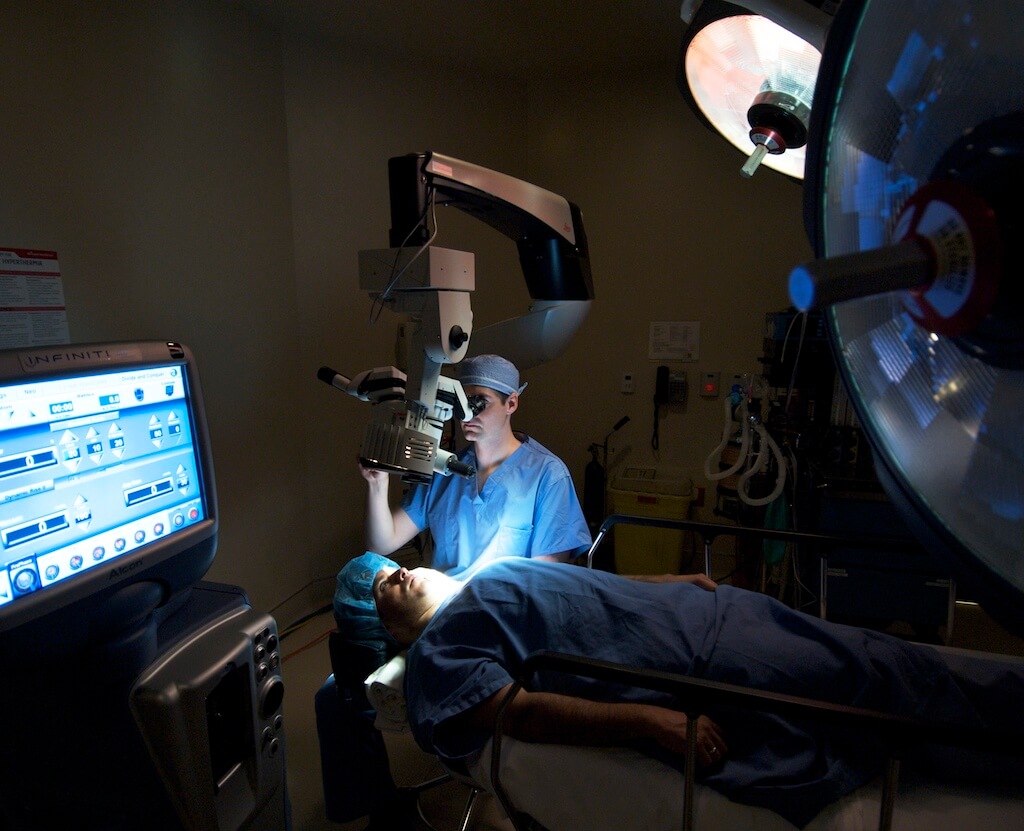
Getting Ready for the Actual Cataract Surgery
Today we continue our line-by-line evaluation of a typical cataract surgery operative report:
The patient was transported to the operating room in a supine position on a Stryker gurney.
This just means that the person about to have cataract surgery is lying face-up.
Once in the operating room, Tetracaine 0.5% drops were placed in the left eye following which Xylocaine 2% jelly was placed in the fornices on the left.
There are many ways to anesthetize the eye. Some doctors give an injection behind or beside the eye. However, this has risks associated with it which include perforating the eye (rare, but more likely in someone who is very nearsighted), bleeding, damage to the optic nerve, etc. For this reason, I prefer a ‘topical’ anesthetic. Anesthetic drops are placed on the eye for immediate anesthesia following which a gel is placed between the eyelids and eye in order to obtain a longer-lasting effect. The drops and gel do sting for a few seconds after they are placed in the eye, but there should not be any pain during the cataract surgery.
The microscope was moved into position and the patient was asked to look at the microscope light which she was able to do without difficulty.
Under topical anesthetic, movement of the eye is possible (indeed, preferred). This can be used to my advantage as a surgeon to direct the patient to look in a certain direction. However, if the patient cannot tolerate the bright microscope light then it might be best to give a retrobulbar or peribulbar injection of anesthetic (mentioned above). The benefits of giving an injection are that the anesthetic lasts longer and the eye is ‘frozen’ (meaning it cannot move during the surgery).
The microscope was moved out of position and the patient was prepped and draped in the standard sterile fashion using a povidone-iodine solution over the left face and lashes and a Betadine 5% ophthalmic solution in the fornices followed by a sterile saline rinse.
Prior to surgery the area around the eye must be cleaned, or ‘prepped’ using a Betadine solution to kill any bacteria on the skin (this helps to prevent infection). A dilute Betadine solution is also used to kill bacteria on the surface of the eye after which it is rinsed out using a salt solution or sterile water.
Steri-Strips were used to drape the lashes out of the operative field, following which Tegaderm was placed over the left face through which a lid speculum was placed.
One of the most commonly asked questions I hear is ‘How will I keep my eyes open during surgery?’ This is the answer to that. A sticky drape acts like scotch tape to keep the lashes away from the eye following which a device that looks like a bent paperclip is used to keep the eyelids open.
Now we are almost ready for surgery. In the next post we will actually get down to the business of surgery.
© 2009 David Richardson, MD





can you be put asleep in this surgery?
Although it is possible to put someone under general anesthesia for cataract surgery, it is rare that we need to do so. The anesthesiologist that I work with is a master of making people comfortable. In general, even the most anxious person can be relaxed with the right cocktail of medications, assurance, and light music. Sometimes people do fall asleep during the surgery. Just last week I had one of my most anxious patients describe the experience as “the most relaxed I’ve been in years!”