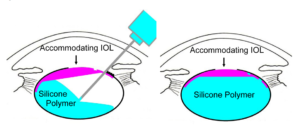
Ref: Nishi O, Nishi K, Nishi Y, Chang S. Capsular bag refilling using a new accommodating intraocular lens. Journal of Cataract & Refractive Surgery. 2008;34(2):302-309.
Modern cataract surgery has come a long way from the days of “couching” (an ancient surgery that essentially involved sticking a needle in the eye and pushing the cataract out of the visual axis). Nevertheless, modern surgeons still worry about the most devastating complication of cataract surgery: post-operative infection, or “endophthalmitis.” Granted, in ancient times this risk was probably quite common. Today rates of post-operative infection range from 1 in 500 to 1 in 2,000 (depending on the study).
The single largest contributor to risk of infection with any surgery is incision size. The smaller the incision, the lower the risk of infection. With cataract surgery, the larger the incision, the greater the risk that bacteria can enter the eye with blinking. Current cataract surgery requires an incision of only 3mm in length. Now, one might think that an incision size of less than 3mm is pretty small, but there is evidence that if we could get the incision below 2mm it could be truly water-tight keeping bacteria out of the eye.
So, what’s keeping us from doing everything through a 2mm incision? We can now remove the cataract through a 2mm incision safely. The problem is getting a new lens (IOL) into the eye. Presently all lenses must be folded or placed in a cartridge and squeezed through the incision. The smallest incision that we can tire-iron these lenses through is 2.2mm (and that’s pushing it – pun intended).
If only there were a way to get an IOL through a smaller incision…
Turns out there are two material technologies that could be used to place an IOL through such a small incision. I’ve already mentioned the SmartLens material which changes shaped according to temperature.
The other material being researched is a polymer that could be injected through a small incision into the capsular bag (this holds the IOL in position) where it would then “cure” or harden into the correct shape.
There are, however, many technical hurdles that must be overcome prior to implementing this technology. For one, how do we know how much material to place in the capsular bag. Presumably, the more material we place in the bag the stronger the IOL will be. But how do we customize this to the needs of that individual eye?
Additionally, how do we cap off the polymer so it doesn’t leak out of the bag? Finally, there is the issue of cure rate. If the material cures too fast the surgeon won’t have time to make the adjustments necessary for a good refractive result. Too slow and surgeons won’t use it (more on the modern time-constraints of surgery in a later post).
I’d give this technology a high probability of appearing on the horizon, but I’d set that horizon at 5-10 years at least.
© 2009 David Richardson, MD







Leave a Reply